Does herpes need to be treated (first infection)?
Treating herpes simplex symptoms, even for the first infection, may not be necessary. Herpes simplex infections clear up even if no treatment is given. But treating genital herpes can be helpful – particularly if there are severe symptoms. Some people are affected more than others. See below for the rare occasions when it can be serious.
A personal experience of treating herpes
“I had 15 herpes outbreaks in the first year. Not surprising really, as I was working 14 hours days, 6 and a half days a week, living on fast food and lacking sleep. Then a year or two later, I changed my job. Now I could sleep adequately, eat better – and the herpes recurrences slowly dwindled away..
“These days, a person with so many recurrences would have have been given aciclovir. But they didn’t do “suppressive therapy” back then, so I treated the symptoms with Lidocaine anaesthetic ointment. Nowadays, if I feel a recurrence – and they are rare – I use Lomaherpan cream (tiny amount, rubbed well in, about 4 or 5 times a day) and that stops them dead in their tracks. ”
What is the usual treatment for genital herpes?
A doctor may prescribe antiviral tablets to speed up healing and reduce the severity of a first episode. Aciclovir is the most commonly used antiviral drug for treating genital herpes. You don’t need the tablets if the first episode is mild, or if you have almost recovered before you see the doctor. If you get more episodes later on, you will be less likely to be offered with antiviral tablets as symptoms clear up without treatment.
The usual treatment for the first infection is aciclovir 400 mg three times daily – although some doctors are still prescribing aciclovir 200 mg five times a day.
Treating a herpes simplex recurrence
To prevent a recurrence with antiviral tablets, you need to start taking them within 24 hours of noticing the beginning of any sensations. (Or better still, within 6 hours! So have them in your pocket/handbag.)
When you start after 24 hours, it is unlikely that the tablets will have much effect. This is why you should have a prescription or tablets ready, so that you can start to take them as soon as possible – see dosing information below.
If you are getting a lot of recurrences, you could take antiviral tablets daily – see dosing information below. You can now get antivirals pills from the GP without having to pay a prescription charge. Ask the doctor to endorse the prescription with “FS” (free supplies).
Members can ask for our antiviral drug fact sheet – see subscription form. And we offer self-help suggestions too.
What are the side-effects of aciclovir?
You can read the patient information leaflet about aciclovir – the one that comes in the box – here. And there is a version for doctors too which has even more detail. Antiviral medications are generally free of side-effects: they work on virus, to prevent it multiplying, and not on human cells.
Should I be treating genital herpes?
For most people antiviral medicine is not necessary either because their body prevents recurrent symptoms or because they find that adopting a healthier life style makes a difference. See What can I do to prevent frequent recurrences?
What are the reasons for taking antiviral pills for herpes?
We have found there are two reasons for taking antiviral pills:
Some people are unlucky and get frequent recurrences, there are two ways that antiviral tablets can be used: episodic and suppression. And some people want to take antiviral pills to reduce the chance of transmission: they use suppression – see below.
Free prescriptions
You can now get antivirals pills from the GP without having to pay a prescription charge. Ask the doctor to endorse the prescription with “FS” (free supplies). Most antiviral pills are suitable for vegans and vegetarians. See Professional’s page for more information.
What's the dosage for treating herpes? How do I take antiviral pills?
These detailed dosages are taken directly from the experts’ guideline on the website of the British Association for Sexual Health and HIV:
Short course therapy/episodic treatment
This should be started within 24 hours of noticing the start of the symptoms – better still, within 6 hours:
- Aciclovir 800 mg three times a day (every 8 hours) for two days – or
- Valaciclovir (Valtrex) 500 mg twice daily (every twelve hours) for three days – or
- Famciclovir (Famvir) 1 g twice daily for one day
Suppression therapy
People take the tablets daily to keep the virus dormant – perhaps for six months or longer. These are now known to be extremely safe drugs. With regard to aciclovir, it is now considered to be so safe that an annual kidney function test is no longer required for long term use:
- Aciclovir 400 mg twice daily (every 12 hours) – or
- Aciclovir 200 mg four times a day (every 6 hours)
- Valaciclovir (Valtrex) 250 mg twice daily (this dose is not available in UK, so you could take half a 500mg twice a day), or else 500 mg daily – or
- Famciclovir (Famvir) 250 mg twice daily
- If breakthrough recurrences occur on standard treatment, the daily dosage should be increased e.g. aciclovir 400 mg three times daily – i.e. 8 hours apart: perhaps 7 am and 3 pm and 11 pm
Be aware that when you stop a long course of tablets, there may be an outbreak 4 or 5 days afterwards. This is not a sign that future recurrences will be frequent – you will need to wait and see.
Should I take antiviral pills for my herpes?
Antivirals are always an option, not a requirement. Luckily – since humans have had herpes since the beginning of time and antivirals were invented in the 1970s. So the decision whether to take them or not is up to you.
If you choose to take them, you can be reassured that they are safe. Even in early pregnancy, aciclovir has not shown any problems. The compound works on virus, not on humans. It works while it is in the body and is expelled in the urine very quickly. This is why aciclovir tablets are taken at least twice a day (12 hours apart).
Reasons for treating herpes with short course/episodic treatment:
- I can feel when the outbreak is starting
- It always starts at the same time in the month
- I don’t get outbreaks very often, so taking pills daily doesn’t make sense to me.
Reasons for choosing suppression/prophylactic/long-term treatment when you have been diagnosed with genital herpes:
- I get lots of outbreaks
- Outbreaks happen without any warning
- I’m worried about passing it on so I want to be sure of not having outbreaks
- While on holiday I want to be sure of not having outbreaks for the two weeks.
- See section above for the dosing.
Aciclovir suppression doesn’t work for me. Help!
If breakthrough recurrences occur on standard treatment, the daily dosage should be increased to aciclovir 400 mg three times daily – i.e. 8 hours apart. This dosage is approved by the expert doctors of BASHH. You can carry on at that dose for as long as you need it.
I get herpes symptoms when I stop taking aciclovir. Help!
Be aware that when you stop a long course of tablets, there may be a recurrence 4 or 10 days afterwards. (A ‘bounce back’ outbreak.) This is not a sign that you will get frequent recurrences in future – you will need to wait and see.
Treat these symptoms either with a ‘short course’ of antivirals (see above) or a cream (see Lomaherpan).
Can a vegetarian/vegan take antiviral pills?
Most antiviral pills are suitable for vegans and vegetarians. See Professional’s page for more information.
Advertisements :
There are now UK-based websites, such as MedExpress and Dr Fox pharmacy which are regulated services, that can supply aciclovir online for treating genital herpes and cold sores, with fast delivery. Only use websites of services registered with the Care Quality Commission (CQC) or the General Pharmaceutical Council (GPhC). Read the NHS advice for buying medicines online.
Any website that is promising “a cure to eliminate the virus from your body” is lying. Currently this is not possible, though there is some interesting research.
Are there side effects from treating herpes with antiviral drugs?
Antiviral drugs are very well-tolerated by most people because they target the virus, not healthy cells. Side effects are rare. Specialist guidelines state that regular kidney function tests for people taking aciclovir long-term are no longer required. The drug has now been used for without problem for over thirty years treating genital herpes. It can be used in pregnancy, indeed it is even recommended that women take it from week 32. See our pregnancy page.
What can I do to stop discomfort and speed up healing? Self-help for genital herpes – first outbreak
People with genital herpes have reported to us that these ideas have helped them to treat their genital herpes. They have not been through a medical trial:
- If required, take a painkiller, such as co-codamol, ibuprofen, paracetamol or soluble aspirin – they reduce pain and inflammation. (Always follow manufacturers’ instructions.)
- Wash your hands before (as well as after) touching blisters or sores, such as when applying medication, as this can introduce bacteria and delay healing.
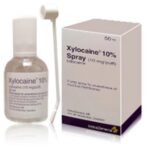
- Apply a local anaesthetic. One of these is lidocaine 5% ointment. It can be used on genital or facial sores. Some people prefer a stronger anaesthetic such as Xylocaine 10% spray. Dab on (or spray on) as required to relieve pain, especially before urinating – see below. (These items are all available from a pharmacy without a prescription – but you will have to ask for them. If the pharmacist says you need a prescription, ask him/her to “check the book” . You do not have to tell him/her what you want it for. Phone us 020 7607 9661 if you cannot find it.) There is a low risk of a negative reaction from topical anaesthetics. If you find that soreness increases, stop using them.
- Keep the sores moist, you can apply Vaseline (petroleum jelly).
- Keep the area clean: washing gently once a day is sufficient. Many people have found a warm salt water solution (1 teaspoon to 1 pint water) very soothing. Gently bathe the area using cotton wool.
- Avoid scented soap and deodorants. It is best not to use wipes, gel or soap in this area, but if you do, use an unscented brand.
- Avoid over-washing as this can increase irritation and delay healing.
- Dab dry carefully with a tissue after washing or use a hair dryer set at ‘cold’.
- To reduce itching, keep the area as cool as is practical: apply a well wrapped ice pack for up to 90 minutes. DO NOT put ice directly on the skin.
- Women who experience pain when urinating during a first episode can try doing it in the bath or shower, or sitting on the edge of the bath and pouring water over the area. This will dilute the urine and ease discomfort. Or try urinating through a tube or into a bottle to prevent urine coming into contact with the sores. You can put lidocaine ointment on the area about 15 minutes before urinating to anaesthetize the area, or use Vaseline (petroleum jelly) or Orabase on the sore as a barrier.
- Do not over-treat the sores – let the skin heal. Symptoms will heal with or without treatment. Beware: Many websites advertise fake ‘treatments’ or even ‘cures’. They may include testimonials and statements by people who claim to be doctors. They are scams. Do not be fooled.
I sometimes get tingles and pains around my buttocks or down one leg. What does this mean?
Occasionally, herpes simplex virus can cause ‘burning skin’ sensations, deep aches or sudden twinges in the genital area. When they occur in the thighs or buttocks, they are sometimes compared to ‘sciatica’. These symptoms are called prodromes – or prodromal symptoms. They are a sign that the virus is trying to reactivate and there may be virus on the skin surface. Sometimes sores will follow, but very often your immune response overcomes the virus before visible signs appear. When you subscribe, to get the email or posted version, you can access more information on treating genital herpes: “Tips to prevent recurrences.”
What are recurrences of herpes and how likely are they?
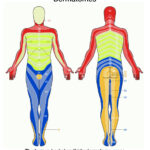
Recurrences (also called outbreaks, episodes, flare-ups) are repeat symptoms (sores, blisters, patches of red skin or tiny splits) which appear at or close to the place where the infection was first noticed – in the same dermatome (see image right). These are often fairly minor and may be no more than a small spot that heals in a few days. They may be accompanied by sensations – itches or nerve twinges. They are unlikely to be as severe as first symptoms and may be almost unnoticed.
They can only happen in the affected area – shown by one colour in the dermatome map. So a genital infection could possibly appear on the anus, buttocks, back of legs – although this is rare.
Does everyone get herpes recurrences?
Around half the people diagnosed only get symptoms once so do not get recurrences – you have to wait to see what happens to you. Recurrences may occur several times a year or can be much less frequent. They usually get milder, heal faster and happen less often as time goes by.
What can I do to prevent frequent herpes recurrences?
There is no need to change your lifestyle or take steps to prevent recurrences until you know whether or not you are going to get any. You will see plenty of internet sites offering dubious ‘treatments’ that are unnecessary and probably have no effect for treating herpes.
These suggestions to help control symptoms come from people with genital herpes, based on their own experiences. The HVA cannot confirm that any of them will work for you, but we believe they are worth considering:
- Try not to worry: worry or stress is known to affect the immune system and lower our ability to fight infections. As you learn more, you will be able to put your diagnosis in perspective and worry less. Your immune system will benefit from this and you may get fewer flare ups. (Stress can also be a trigger factor for many other skin conditions, e.g. eczema, psoriasis.)
- Get enough sleep and avoid getting too tired.
- Eat a well-balanced, healthy diet with plenty of fruit and vegetables.
- Take a modest vitamin E supplement (200 i.u. per day). This has been shown to boost immune response.
- Try to avoid causing soreness to genital skin. ‘Skin trauma’ caused by waxing, shaving, thongs, tight trousers, horse or bike riding or even sexual activity may trigger a recurrence. See suggestion in the section on ‘prevention’ below. Talk to the helpline on 0845 123 2305 if you need advice about these.
- Give up smoking or try to reduce it, and cut down on excessive drinking.
- Take regular exercise: 20 minutes brisk walk each day is a good start. But too much exercise can tax the body so that it doesn’t ‘have the energy left’ to work at controlling the virus.
- Try taking one soluble low dose aspirin each day with food. (For adults only. This is not recommended for people with stomach problems. Talk to your doctor first.)
- We have tested various herbal products designed to help your body control the virus. Two that we found effective are shown in our shop page. Two thirds of the people taking these in our trials reported a good result: fewer, shorter or no recurrences! (Any advertisement that says their product is 100% effective is lying.) If you can, buy two tubs of either one, as the trials showed that you need to allow time for these to work.
- If sex is a trigger try using silicone based lubricant (this is sold to enhance pleasure). You could use this if bicycle or horse riding triggers your recurrences. However, this is problem for very few problem.
- Avoid direct sunlight or ultraviolet rays from sunbeds on the site of infection, i.e. no nude sunbathing! If you have cold sores (facial herpes simplex), use a sunblock to protect your skin.
- Join SPHERE and ask for the ‘Tips to Prevent Recurrences’ – two sides of A4. Sample issue of the magazine can be read here.
- Talking to someone else who has personal experience of herpes simplex can be helpful. Join the HVA, come to meetings and/or call our helpline: 0345 123 2305. Experience, advice, understanding and useful information are just a call away.
- Come to a London drop-in session hosted by one of our volunteers – they are informal and open to all – see Events page .You will see plenty of internet sites offering dubious ‘treatments’ that are unnecessary and probably have no effect. Our “Tips to prevent recurrences” is a two-page list of self-help suggestions for treating genital herpes. We also produce leaflets on “Stress”, “Boosting Immunity”, and reports of our trials on “Olive Leaf Extract” and “Eleutherococcus senticosus” (Elagen). Members can order these leaflets when they join.
Is there a cure for herpes?
No, there is no cure for herpes simplex virus at present. None of the advertisements that advertise a “guaranteed 100% cure” are verifiable. Don’t fall for these scams.
We are following the research that is being done now with interest. Herpes research is mostly being done in the USA. The charity’s journal for subscribers reports on all this research. Sometimes, it is important enough to be added to our News page.
There are plenty of internet sites offering dubious ‘treatments’ that are unnecessary and probably have no effect. Our “Tips to prevent recurrences” is a two-page list of self-help suggestions for treating genital herpes. We also produce leaflets on “Stress”, “Protecting your Immune System”, and reports of our trials on “Olive Leaf Extract” and “Eleutherococcus senticosus” (Elagen). Members can order these leaflets when they join.
If you read on the Internet “Buy my cure for herpes” “Guaranteed cure for herpes 100%.” These are lies. Anyone can write that this has been developed/proved by doctors and that there are 3 million satisfied customers. This is not necessarily true!!!
The best these treatments can do is improve your immune function so that your body does a better job of controlling the virus and we have lots of ideas for this. See above.
Subscribe to get SPHERE – our magazine. In each issue there will be articles about research, trials etc. Sample issue of the magazine can be read here. You can see a list of articles published in previous magazines.
Tell us what you think of this website
Help for you
You can phone the helpline on 0345 123 2305, or email us at [email protected]
Help for us
We are not funded by NHS or government. We rely on your donations to continue. Please donate!
This page was updated on 8-1-2026




